
Words by Julie De Vos | Photos by Mike Last
Part One: Diabetes Management
We all envision our race day to be 15 degrees celsius partly cloudy with a very light breeze – the PERFECT running day! In reality, we’re lucky if our actual race day is as perfect as our envisioned one. Maybe it’s because during the colder temperatures and less than ideal weather we take to the treadmill and we forget just how much the weather affects our diabetes management.
With or without diabetes the weather plays a role in how we perform and planning correctly can make or break your training day or your actual race.
In this first blog of the two part series we’ve compiled some tips for managing different weather situations and their effects on our diabetes.
Cold Weather

Cold weather tends to drop our blood glucose levels as our bodies are working hard to keep us warm. Whatever your management plan whether it’s cutting back insulin or eating extra carbohydrates, your body is working even harder. Planning for this can help reduce lows during and after exercise.
- Make sure to bundle up in layers. As you get further into your run your may notice you start to get too hot, wearing layers allows you to take something off to maintain a happy body temperature.
- Don’t forget your hands and feet! Wearing light gloves and warmer socks will help protect your fingers and toes. Cold fingers are tough to get blood from!
- Keep your meter and other technology warm. Keep it in an inside pocket close to your core. Most meters will give false readings outside of their operating temperatures. If your meter isn’t working, try warming up the batteries in your hands or in your armpit (hey, it’s warm in there!).
- Just because it’s cold out doesn’t mean you don’t sweat. Remember to stay hydrated before, during, and after your run.
Hypothermia – it can happen in warmer weather too

Hypothermia sets in when your body loses its heat faster than it can generate heat, which can cause a low body temperature resulting in a medical emergency.
According to the Mayo Clinic, “normal body temperature is around 98.6 F (37 C). Hypothermia occurs as your body temperature passes below 95 F (35 C).”
- How can you get hypothermia? It’s often due to inadequate preparation for unanticipated exposure. Some examples of situations that may lead to hypothermia include being caught in a winter storm, a car accident or an outdoor sports enthusiast caught off guard by the elements (ie sudden downpour of rain).
- Hypothermia doesn’t just occur in cold temperatures! Being caught in the rain without rain gear and high-velocity wind exposure are two ways in which hypothermia can sneak up on you in warmer temperatures. Always be aware of your climate surroundings.
- Remember: Keep protected from the elements and stay dry!
Rain– spring has sprung!

As our weather turns warmer and the season changes, we can count on one thing: the wet weather.
- The aim of the game is keeping dry – you and everything you’re carrying.
- Little zip lock baggies work wonders and can keep your items dry in a pinch.
- Getting wet can lead to cooling of your body temp. Watch out for accidental hypothermia.
Wind– easy, breezy, beauti…err…happy runner?

Often times in warmer weather a light breeze can make a huge difference between being overheated and just right. However, the wind can also cool us down more than we’d like through a process called convection.
- What is convection? As the cold air moves across exposed skin our internal temperature is cooled. This is how a ceiling fan works to cool us down.
- Keep covered up, even with a light long sleeved shirt. You may also want to wear a hat or beanie to keep heat escaping from your head.
Warmer Weather– out of the deep freeze & into the frying pan
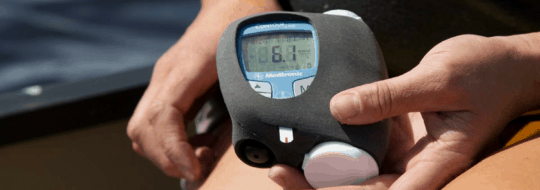
Warmer weather may cause a change in your insulin needs, while the reason for this is not exactly understood, we do know that higher temperatures may change how your body uses insulin. Be sure to check your BGs often.
- Keep yourself hydrated– drink plenty of water, especially in the hours leading up to a run, during, and after. It’s important to stay hydrated throughout the day, not just during exercise.
- Dehydration can lead to a rise in blood glucose levels and increase the likelihood of developing ketones.
- Protect your diabetes gear – heat and direct sunlight can damage your blood sugar monitor, insulin pump, and other diabetes equipment (such as test strips).
- Wear loose-fitting, lightweight, light-colored clothing to help keep your body cool.
- Wear sunscreen and a hat to keep the sun off your head and out of your eyes. Sunburns can raise your blood sugar levels.
- Watch out for muscle cramping as it might be the first sign of heat-related illness, and may lead to heat exhaustion or heat stroke.
- If you feel weak or light headed, remember to stop, drink some water, and head to a cooler area to rest. We’ll discuss heat related illnesses and what to do in an upcoming blog
Humidity

Your body self-regulates your temperature by sweating, which cools you as it evaporates from your skin. Because the air itself is damp when there’s high humidity, it can be harder to stay cool since your sweat doesn’t evaporate as well.
Because of the increase in moisture in the air (and on you) there is a higher likelihood that pump sites and CGM sensors will have difficulty adhering to the body. Try some skin tac before inserting or some extra tape if you’ve already inserted.
As with any exercise, remember to test and test often. Let a friend, family member, or spouse know where you are going running and for approximately how long you’ll be gone for.
Sources:
- https://www.cdc.gov/features/diabetesheattravel/
- http://emedicine.medscape.com/article/149546-overview
- http://www.mayoclinic.org/diseases-conditions/hypothermia/basics/definition/con-20020453
- http://emedicine.medscape.com/article/770542-overview?pa=Q9PgHHtrclKswyasPMWmFBTJjzoKhXZUsD5pborpkH9KW%2BrgepMvO7swoK4ms1SbcxxkiIPHfaTFdnS1zGRg3%2FEiL5fM42L%2B9xlMlua7G1g%3D
- https://www.cdc.gov/extremeheat/warning.html




